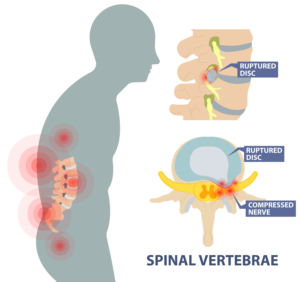
What is a ruptured disc?
Firstly, what are we talking about when we say disc? There are discs in your spine that are found in between vertebrae which help with maneuvering the spine and act as shock absorbers for these movements. Spinal discs rupture due to a fall, car accident, sports injury or some other type of physical impact involving the spine. However, aging can cause disc degeneration, which heightens the risk for a disc to rupture. If the discs dehydrate and weaken over time the outer walls of the disc can bulge and rupture allowing the inner nucleus to protrude onto the surrounding nerves.
Ruptured Disc in the Back
Pinched nerves in the back due to a ruptured disc can cause pain in the back, but this alone can be caused by a number of other conditions like muscle strain. When pain in the lower back is paired with a radiating pain down one or both legs this is much more likely to be caused by a ruptured disc. Ruptured disc in the back are usually called lumbar herniated discs.
Ruptured Disc in the Neck
When a disc rupture happens in the neck it’s called a cervical herniated disc. The resulting neck pain is associated with arm pain, numbness and tingling. The pain can also radiate down to your hand and cause weakness in the arm and hand. This can result in difficulty grasping objects, or performing small mechanical actions like buttoning a shirt. The pain also flares up when turning your head or bending your neck, and possibly resulting in muscle spasms.
Ruptured Disc Symptoms
There are a number of common symptoms that indicate you have a ruptured disc. Generally if you have a ruptured disc you will experience:

- Pain in the back or neck
- Numbness to one side
- Radiating pain down an arm or leg
- Pain that worsens at night
- Increased pain if walking or sitting
- Muscle weakness
- Tingling or burning sensations
- Pain with certain activities like bending or lifting
If you have many of these symptoms it’s best to consult with a doctor to ensure you can resolve your symptoms. Sometimes ruptured discs heal on their own with rest and little medical intervention. However, a ruptured disc can also get worse over time. Doctor’s can come up with a plan to make sure your rupture disc doesn’t get worse, and give recommendations about treating the pain, symptoms, and healing the disc.
Treatments for Ruptured Discs

In order to treat ruptured discs your doctor must achieve an accurate diagnosis. The first step in diagnosing this condition is to do a physical examination by checking your back or neck for tenderness, and how certain movements affect your pain levels. Your doctor will also go over your medical history. Usually these processes are enough to conclude a diagnosis of a ruptured disc, but in some cases an imaging test may be needed to clarify which nerves are affected or to rule out other conditions.
Basic treatment for a ruptured disc include resting to give your spine time to heal, and avoiding any intense physical activities or things that cause exertion to your back. Though you will want to keep some very light activity and not be completely bedridden during the process, as some activity promotes healing. Pain medications help control the pain caused by a rupture disc and reduce inflammation and swelling. Ibuprofen or naproxen are common over the counter pain medications that are useful during the recovery process, and if needed there are cortisol injections that are more targeted treatments for pain management and inflammation reduction.
Physical therapy and exercise help improve the strength and flexibility of your muscles, which support your spine and the ruptured discs. Stretching during physical therapy is also an important part of physical therapy as well as aerobic exercises. Ice and heat packs can be applied to the area as well
Ruptured Disc Image Testing
Depending on the conclusions of the physical examination and the need for more testing your doctor may order an X-Ray to view the bones of the spine, or an MRI to view a 3 dimensional image of the internal structures of the spine including the vertebrae, discs, and surrounding tissue. An open MRI is great at examining the spine since it can pin point the location of a ruptured disc, see which nerves are affected, and the extent of the rupture.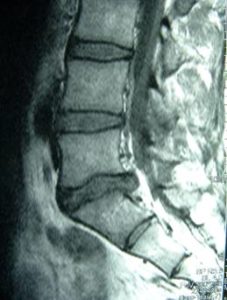
If more testing is required or will aid in better understanding the condition there are nerve tests that can be performed as well. Nerve conduction studies measure electrical nerve impulses and functioning, which are is useful data in identifying any nerve damage. Electrode patches attached to your skin are used to stimulate the nerve impulses. The electromyography is a similar procedure in that it’s used to determine how healthy nerve cells are as well as the muscles surrounding the nerves. A nerve conduction study uses electrode stickers placed on the outside of the skin to measure electrical nerve impulses between two or more points, while an EMG (electromyography) use needles which are inserted directly into the muscle to graph the electrical signals being sent out. All this data is helpful to an expert to determine nerve health, and possible nerve damage due to a ruptured disc.
Ruptured Disc Surgery
In cases that medication, exercise, and rest doesn’t heal the ruptured disc surgery may be necessary. Though many people do heal within 6 weeks with conservative treatments, some symptoms become so severe they can interrupt daily life. If your symptoms are worsening over time or you have trouble standing or walking surgery is a viable treatment option to help heal the ruptured disc. There are a few different types of surgery that can help with a ruptured disc such as the following:
Discectomy
The first type of surgery many people receive is called a discectomy. This procedure involves removing the disc that ruptured and is putting pressure on nearby nerves. Discectomy surgery can be performed using minimally invasive techniques, in which case it’s called a microdiscectomy. The difference is the surgery is done through a significantly smaller incision through a small tube called an endoscope.
Laminotomy
Laminotomy has a similar concept as a discectomy, but instead of removing part of the disc causing pain, a portion of the spinal vertebra called the lamina is removed. The lamina is a protective covering in the spinal cord, but sometimes a nerve can get trapped between the lamina and a ruptured disc, so removing a part of it helps relieve the pressure. It can be performed while a discectomy is performed, or as an individual surgery.
Spinal Fusion
Spinal fusion is a procedure that fuses two vertebra together to help stabilize the spine and prevent any more pain and injury to the area. The process for this surgery involves grafting a bone between the two vertebrae and securing the bone graft in place using metal plates and screws to allow the graft to beside the bones and permanently fuse them together.
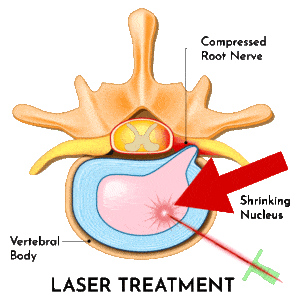
Laser Spine Surgery
Laser surgery for the back is a minimally invasive alternative to spinal fusion and discectomy. The procedure shrinks a ruptured disc, relieving the pressure on nearby nerves and allowing the disc to heal. There is no cutting required, since the laser is fed through a needle directly to the ruptured disc, allowing the treatment to proceed with minimal risk. Many people find this to be advantageous to other forms of spinal surgery, and enjoy quicker recovery times. Consult with your doctor about your options if you’re experiencing severe back pain or neck pain.


