 What is Ankylosing Spondylitis?
What is Ankylosing Spondylitis?
Ankylosing spondylitis is a rare form of arthritis that affects the spine, though it can start affecting other joints as well. The inflammation within the spinal joints causes pain, discomfort and in very severe cases, fusion between spinal vertebra. Other parts of the body that may experience inflammation include the shoulders, hips, ribs, heels, and the hands and feet. One of the primary joints to be affected is the sacroiliac joint as the disease progresses. SI joints are where the spine joints the pelvis, and generally don’t have a great deal of movement.
Ankylosing Spondylitis Diagnosis
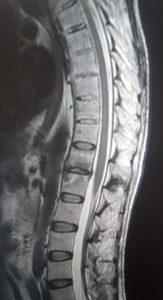
Diagnosing ankylosing spondylitis is a multi step process which starts with a physical exam. Many people walk into a doctors office complaining of back pain, so it can be tricky diagnosing AS since there are a great number of causes of back pain. Your doctor may ask you to bend to see what your range of motion is with your spine, and may try to see what is producing your pain by asking you to move your legs in a certain position, or pressing on parts of the body. Your doctor can also ask you to take a deep breath to check if you have difficulty expanding your chest. If your doctor suspects you might have ankylosing spondylitis an MRI is the next step in diagnosing accurately.
Open MRI machines, also known as magnetic resonance imaging, use extremely powerful magnets to produce strong magnetic fields. This combined with a radiofrequency current pulse creates a 3D image of the spine and surrounding tissue. It’s very accurate, and since it doesn’t use radiation or require contrast dye to be effective it is a safe diagnosing test with very few risks or complications. The detailed image can see the more subtle clues of ankylosing spondylitis so your doctor can spot the disease early on.
 Causes of Ankylosing Spondylitis
Causes of Ankylosing Spondylitis
People aren’t sure of the exact cause of ankylosing spondylitis, but one theory is that it’s genetic. Most patients with AS have a gene in common that produces the HLA-B27 protein, and it may be this gene that causes the onset of ankylosing spondylitis. There are also some slight risk factors such as sex and age. Men are more likely to develop AS and also a more damaging version of the disease. Women usually develop a form of AS called non-radiographic axial spondyloarthritis, which symptoms aren’t quite as bad. Age is also a factor, as in most cases it develops in a patient’s teens and young adulthood, with 80% of cases beginning before the age of 30.
Some of the Symptoms of Ankylosing Spondylitis
Since ankylosing spondylitis starts with the sacroiliac joints there are many primary areas you may feel pain or stiffness. Those being pain in the lower back, buttocks, shoulders, hands, hips, thighs, feet and heels. You’ll probably feel the pain and stiffness in your lower back and hips first though, particularly in the morning or after intense activity. You may also experience neck pain and fatigue.

Treatments for Ankylosing Spondylitis
There are many kinds of treatments for ankylosing spondylitis, which will vary depending on the severity of symptoms, overall health of the patient, and any existing conditions or medications. Managing ankylosing spondylitis starts with exercise and physical therapy. The more active you are the more your spine can be supported by strengthened muscles and keep you aligned standing up straight. Exercise is a powerful tool for getting rid of spine pain, but it’s important to be mindful of form, and not to overdo it and cause more damage to your spine. Working with a physical therapist is great since they can guide you on exercise routines, stretching for the spine, maintaining good posture and other techniques to keep the lower back pain at bay.
Medications for Ankylosing Spondylitis
Nonsteroidal anti-inflammatory medication can help control the inflammation that AS causes. Prescription strength medicines like naproxen or indomethacin can help control the symptoms of ankylosing spondylitis, but may have side effects such as stomach bleeding, heart problems and others. There are other medications called biologics like TNF blockers (tumor necrosis factor) that target a protein causing inflammation in the body. They help reduce pain, stiffness and tender / swollen joints, and are injected under the skin or through an IV. However, they can make you more prone to infection, or reactivate untreated tuberculosis.
Corticosteroids for Treating AS
Corticosteroids can be take orally or as an injection to treat ankylosing spondylitis and permit a strong anti inflammatory response. The injection can be administered directly into the inflamed joint and can have longer lasting effects than other pain management medication. There shouldn’t be more than 3 corticosteroid injections in a year due to the possible side effects. The risks include infection at the injection site, skin changing color at the injection, and a tendon near the joint bursting.
Surgery for AS
Much of the time patients who have ankylosing spondylitis will not require surgery, but if the hip joints have become severely damaged over time there may be a recommendation for hip replacement. Another case where surgery might be necessary is if the spine starts to become bent after experiencing AS symptoms for a period of time, though this is more rare. You’ll want to see a rheumatologist or general practitioner to monitor your condition and see how treatments are working or if your condition is progressing.


